Over the past 6 years I have published several articles on the need to personalize health insurance (and get the employer out of the way) by making an individual insurance policy tax deductible. This happened partially through the introduction of the Individual Coverage HRA (ICHRA) which was effective January 1, 2020, but it did not go far enough. Since the ICHRA became effective I have analyzed 50+ employers across the country comparing their group health insurance program to alternatives on the individual market. While not all individual markets are competitive at this time, I have seen enough evidence to conclude that the move to a total individual insurance market is inevitable and it could happen with one quick stroke of the pen. The benefits of this change can be tremendous. Employees throughout the U.S. will reap benefits through lower costs, more options, and ultimately better health care.
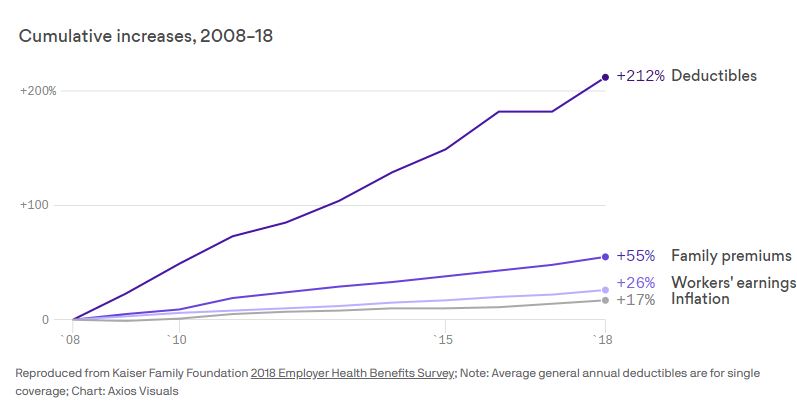
The running narrative around employer-based insurance is that it is not broken. I disagree. An interesting statistic, that few in the business have realized, is that the number of employees covered under employer-based insurance is the same today as it was in 1998 while the population has been rising. (Source: Kaiser) Deductibles and employee contributions have also increased at rates higher than inflation and wage growth, creating a working poor population. (See chart below) I do not know how many more non-profits or home health care companies I need to look at that have 30% participation to support my position.
I have recognized a few things while analyzing the 50+ cases. First, I will say that employers are over-buying insurance for most employees. One size does not fit all and many employees, when given options, would choose more narrow networks with slightly higher deductibles and fewer pre-deductible copays if they can benefit from the decision. In Massachusetts, the average individual insurance buyer is choosing a plan that is 14.4% – 33.7% less expensive (depending on income) than the average large employer. (Source: MA Health Connector) This frees up an average of $2200 per year that can go towards a health savings account or maybe pay down one’s credit cards. Employers are forcing employees to pay more for health insurance leaving less money to pay for actual health care. Funding an HSA will make money available for first dollar care.
Another issue I am realizing, though I will not get into all the details here, is that the majority of the “decision support tools” guiding employees current buying decisions through employers are flawed. This is a big statement that will get some pushback. I will cover this in another article and back it up with data. My only point here is that these tools are also contributing to consumers over-buying insurance. Few who are buying health insurance have a true understanding of their real risk.
The current model of group insurance is a one-size fits all model. The employer buys one or a few options and asks employees if they want to participate in this employer purchased insurance. I have to ask, where in our personal lives does one size fit all? Everything is becoming personalized. Consumers, when acting in their own best or selfish interest, can make decisions and drive down costs. The employer in the middle is the problem.
Another belief is that employers have more buying power than an individual. That really is not true. Individual insurance is negotiated with the States and the individual market is one big risk pool. In most States insurance companies have tens of thousands of employees in their individual risk pools underwritten as one big group. Also, when one looks at the cost of running an individual program it is often 5-6% less than running a typical group program.
The current market depends on two things to “release the power of the markets”. First it requires the employer to “give employees the freedom to choose” by adopting an ICHRA. The second is the health insurance companies need to rethink their position on the individual markets. States can also lead the way by adopting the MA model of pricing health insurance. I have looked at all 50 States and MA has it right. In Massachusetts, individual and group pricing are required to be priced as one risk pool. In prior articles I have written that splitting risk pools is a key cause of the problems with the U.S. health insurance system. By putting individuals and groups in the same pool it stabilizes the markets and stops the gaming of the system by employers seeking better risk pools. For those thinking the that employers managing risk through all types of crazy cost containment programs is something they want to do I would argue that most would prefer to simply be out of that business.
This gets to my prediction, and a possible solution to saving the private health insurance markets, driving down costs, and ultimately improving consumer health care. Through Executive Order, the President (whoever it is) can make an individual insurance policy an eligible expense under a Health Savings Account. By doing this the employee could be in control, not the employer. An employee can ask the employer to pay them the money instead of buying their health insurance, giving the employee the option to buy what they want. The insurance companies would respond to this new demand and start focusing more on the individual market. Capitalism and market forces can work, if we let it.
This change could happen under a Trump or Biden Presidency. Trump has already indicated that he intends to expand options. Secretary Alex Azar said in September 2020 that, “We’ve created new ways for workers to have a broader set of insurance options through Health Reimbursement Arrangements, and the president pledged last week to push for more reforms to open up even more options.” These more options could be the Health Savings Account.
Biden’s big push is for a Public Option. I would assume the Public Option is chosen by individuals not employers, so he would be in favor of maintaining the ICHRA rules and possibly expanding individual choice. I want to add that I really do not understand the deal of the Public Option. If the hospitals and doctors would accept Medicare type reimbursements right now from any insurance company, they could do it without the government being involved. The Public Option could be run through a private market today if the providers would accept lower reimbursements from private plans. The current problem is the providers need the private markets to subsidize public plans. This may play out soon.
The move to a consumer-centric model based around individual health insurance is inevitable. I think employers, employees, and providers would welcome the change. It is an easy change because the individual health insurance markets and Health Savings Account Administrators already exist. Much like the ICHRA, with one stroke of the pen, tens of millions of Americans can be choosing their own health insurance in 2021. Employers can provide money to employees for health insurance as they are today, but when it comes to choosing health insurance they simply need to get out of the way.

Thanks.
I too like the idea of greater individual control. However, not sure most employees who have employer-sponsored coverage today would agree.
If I understand your proposal, you want to decouple the requirement of employer-sponsored HSA-capable coverage from employer contributions to Health Savings Accounts (and, I assume, employee pre-tax deferrals via a cafeteria plan). I assume you plan to expand the Health Savings Account contribution maximum from $3,600/$7,200 (2021) to a much higher number (so as to accommodate both premium and out of pocket spending, and to facilitate accumulation of assets). Some questions:
I assume that plan to retain the employer mandate but allow it to be satisfied by some dollar amount of contribution to a Health Savings Account?
Or, did you decide that employers no longer need to contribute towards the cost of health coverage – only that employers are mandated to maintain a cafeteria plan that allows for pre-tax contributions to a HSAs (sort of like the Massachusetts Connector)? Or, did you expect that employer contributions to the HSAs (and employee contributions as well) would be imputed as income or deducted after-tax? That would raise a lot of revenue and more than replace the budget hole Congress created by repealing the “so-called” Cadillac Tax.
Does your proposal anticipate higher employer contributions for some workers and not others – making explicit what is already commonplace for:
– Older workers, compared to younger workers, someone age 60+ costs perhaps 5x what someone <25 costs, on average (and averages can be deceiving), and
– Workers who elect to cover a spouse and/or children up to age 26, compared to workers who waive coverage for themselves, or a spouse and/or children?
For those who have a spouse or adult children who have access to coverage through a spouse's employer, what contribution would be appropriate in such a situation?
And, what about those who have a spouse or dependent children but prefer coverage under a spouse's employer's plan? Are you proposing eliminating all employer-sponsored coverage, or perhaps eroding it quickly by eliminating the tax preferences for employer contributions?
And, won't exposing all these flat dollar amounts of employer contributions (or worse, those who contribute more for lower paid workers by using a progressive scheme) highlight the disparate treatment where employer financial support for lower compensated employees is disproportionately higher (as a percentage of total rewards, and perhaps relative to their contribution to results) when compared to that of higher compensated employees?
Many employers hide all of these disparities from themselves in their budgeting processes. Once exposed … will they change strategies?
And, should we assume that those receiving an employer contribution to the Health Savings Account will be ineligible for the taxpayer financial support in exchange coverage?
Thanks for repeating the chart from the Kaiser study. Yes, deductibles have increased 200+% (their number) over the past ten years. Kaiser confirms in their most recent edition (2020) that: "… For covered workers in a plan with a general annual deductible, the average annual deductible for single
coverage is $1,644, similar to the average deductible ($1,655) last year. …"
However, if you go way, way back 35 years, when the average deductible was ~$200, and compare the increase in deductibles with that of premium (in terms of impact on take home pay), you'll see deductible increases have been much less.
Let us know the specifics.
LikeLike
You obviously asked a lot of questions and the answers would be more in a book versus an article. I had written on this in past blogs. (The Coming End to the Health Insurance Business as We Know It – And What Brokers Can Do About It) One thing I am convinced of is that easy access to capital from a third-party, such as in health insurance through employers and education through easy loans, is an inflationary formula. I think most people would agree with that. I also think employers would prefer to get out of the health insurance business. They will need to give people money to compete for talent and some of that money can go to pay lower health insurance costs.
Here are quick answers:
– The employer deduction should go away and it should move to the employee but that would take action by Congress. Step 1 is through an HSA because this can go through Executive Order.
– The HSA limit would have to be raised.
– Everyone should participate which is why we need individual choice and the need to drive down costs.
– Employers will have to compete for talent and therefore continue to make contributions.
– Contributions can be age, family status, and location based. We are doing this today with ICHRA’s.
– Employees can contribute through payroll deduction
– If everyone can buy individual insurance employees and spouses can buy independently or together. It really shouldn’t matter.
– In time the law would allow a deduction for all individually purchased insurance but it would be progressive not the current regressive nature of the deduction.
– Other problems not referenced that go with job lock and disconnected health insurance and health care are big problems with employer-based insurance that continue to be swept aside.
I have run numbers a hundred times. I am convinced that a consumer can outperform and employer if they were not handicapped by tax laws. If the government let markets work then everyone will win.
LikeLike